X-linked lymphoproliferative disease (XLP)
2012-04-01 Hamid Bassiri , Kim E Nichols AffiliationDivision of Infectious Diseases, Childrens Hospital of Philadelphia, Philadelphia, PA 19104, USA (HB); Division of Oncology, Childrens Hospital of Philadelphia, Philadelphia, PA 19104, USA (KEN)
Identity
Name
X-linked lymphoproliferative disease (XLP)
Note
Two subtypes of XLP have been idenitified to date.
, XLP type 1, (also known as Duncan disease, Purtilo syndrome) is a rare primary immunodeficiency, first described by Purtilo (Purtilo et al., 1974), in which patients develop dysgammaglobulinemia (most commonly hypogammaglobulinemia of one or more immunoglobulin subclasses), fulminant mononucleosis following infection with Epstein Barr virus (EBV), and B-cell lymphoma. XLP1 is caused by mutations in SH2D1A (formerly DSHP; SAP), which encodes the cytoplasmic adaptor protein Signaling Lymphocytic Activation Molecule (SLAM)-associated protein (SAP) (Coffey et al., 1998; Sayos et al., 1998).
, XLP type 2, (Rigaud et al., 2006) is a clinically similar disorder that predisposes primarily to hemophagocytic lymphohistiocytosis (HLH), which often presents in the setting of primary EBV infection. Patients with XLP2 may also exhibit splenomegaly, hypogammaglobulinemia and hemorrhagic colitis (Marsh et al., 2010). To date, no patient with XLP2 has been reported to develop abnormal B-lymphoproliferation or lymphoma. XLP2 is caused by mutations in XIAP (BIRC4), the gene encoding the X-linked inhibitor of apoptosis protein.
, XLP type 1, (also known as Duncan disease, Purtilo syndrome) is a rare primary immunodeficiency, first described by Purtilo (Purtilo et al., 1974), in which patients develop dysgammaglobulinemia (most commonly hypogammaglobulinemia of one or more immunoglobulin subclasses), fulminant mononucleosis following infection with Epstein Barr virus (EBV), and B-cell lymphoma. XLP1 is caused by mutations in SH2D1A (formerly DSHP; SAP), which encodes the cytoplasmic adaptor protein Signaling Lymphocytic Activation Molecule (SLAM)-associated protein (SAP) (Coffey et al., 1998; Sayos et al., 1998).
, XLP type 2, (Rigaud et al., 2006) is a clinically similar disorder that predisposes primarily to hemophagocytic lymphohistiocytosis (HLH), which often presents in the setting of primary EBV infection. Patients with XLP2 may also exhibit splenomegaly, hypogammaglobulinemia and hemorrhagic colitis (Marsh et al., 2010). To date, no patient with XLP2 has been reported to develop abnormal B-lymphoproliferation or lymphoma. XLP2 is caused by mutations in XIAP (BIRC4), the gene encoding the X-linked inhibitor of apoptosis protein.
Inheritance
XLP1 and -2 are transmitted in an X-linked fashion and do not have a known ethnic or racial predilection. The causative genes are located in proximity to one another at Xq25. Mutations in SH2D1A or XIAP are identified in 83-97% of XLP1 and 12% of XLP2 patients, respectively (Filipovich et al., 2011). Mutations include insertions, deletions of one or more exons and nucleotide substitutions that result in reduced or absent expression of the encoded proteins. De novo mutations in either gene are rare. Female SH2D1A or XIAP mutation carriers are clinically unaffected yet at risk to transmit the mutant allele to 50% of male offspring, who will have XLP. Female offspring of XLP carriers are at 50% risk to inherit a mutant allele and thus be carriers of XLP.
Omim
308240 , 300635
Mesh
D008232
Orphanet
2442 X-linked lymphoproliferative disease
Umls
C0549463
Clinics
Note
XLP is estimated to affect 1-3 per million male individuals, although the incidence may be higher as the condition may go undetected. Nonetheless, any male individual presenting with severe or fatal EBV infection, or HLH as a result of EBV exposure should be evaluated for XLP, especially if there is a family history of maternally related males with dysgammaglobulinemia, lymphoma or EBV-induced HLH. Early diagnosis of XLP is paramount, as the mean ages of death of individuals with XLP1 and XLP2 are 11 and 16 years, respectively (Pachlopnik Schmid et al., 2011).
Phenotype and clinics
XLP1 patients usually present with fulminant FIM (a hyperinflammatory condition resembling HLH that is induced by EBV infection and typified by the dysregulated expansion of EBV-infected B cells and cytotoxic T cells, and the abnormal activation of macrophages), dysgammaglobulinemia and B cell lymphoma. Less commonly, XLP1 manifests as lymphocytic vasculitis (usually involving the lungs or central nervous sytem [CNS]), aplastic anemia or lymphatoid granulomatosis (Gaspar et al., 2002). The manifestations of XLP1 can occur in the absence of EBV infection.
XLP2 commonly presents with splenomegaly and recurrent episodes of HLH, often in response to EBV infection. XLP2 patients also display dysgammaglobulinemias, and a proportion of affected individuals develop hepatitis and\/or colitis.
There is no known correlation between SH2D1A or XIAP genotype and phenotype in XLP1 or XLP2. Affected members of the same family may exhibit significant variability in presentation.
Diagnosis is generally suspected based on clinical history. Screening tests can be performed to assess for protein levels of SAP or XIAP in lymphocytes via flow cytometry, and the diagnosis confirmed by genetic analysis of the associated genes. In rare instances, genetic analysis fails to identify an abnormality in SH2D1A or XIAP in a host presenting with signs and symptoms consistent with XLP.
XLP2 commonly presents with splenomegaly and recurrent episodes of HLH, often in response to EBV infection. XLP2 patients also display dysgammaglobulinemias, and a proportion of affected individuals develop hepatitis and\/or colitis.
There is no known correlation between SH2D1A or XIAP genotype and phenotype in XLP1 or XLP2. Affected members of the same family may exhibit significant variability in presentation.
Diagnosis is generally suspected based on clinical history. Screening tests can be performed to assess for protein levels of SAP or XIAP in lymphocytes via flow cytometry, and the diagnosis confirmed by genetic analysis of the associated genes. In rare instances, genetic analysis fails to identify an abnormality in SH2D1A or XIAP in a host presenting with signs and symptoms consistent with XLP.
Neoplastic risk
The risk for development of lymphomas in XLP1 approaches 25-30%, with a mortality rate of 9% (Booth et al., 2011). The lymphomas are typically high grade non-Hodgkins type B cell lymphomas. Lymphomas tend to be extranodal and involve the intestines, although they can also be found in liver, kidneys and CNS. Histologically, they are classified as Burkitts, immunoblastic, small cleaved B cell lymphomas or mixed cell lymphomas. Not all lymphomas carry evidence of EBV genome. It remains poorly understood why patients with XLP1 develop lymphoma; however, absence of invariant natural killer T (NKT) cells and defects in T and NK cell cytotoxic function may contribute to lymphoma formation.
Treatment
The therapy of choice for XLP patients is hematopoietic cell transplantation (HCT). HCT is the only known curative treatment and has the best chance of success if performed as early as possible - before the onset of other disease manifestations. Other therapies directed at treating the manifestations of XLP may be necessary before HCT is attempted. Although HCT carries its own risk of complications and mortality, without it only 50% of XLP1 patients reach adulthood. The majority perish secondary to HLH (70%), lymphoma (12%) or myelodysplasia (6%) (Booth et al., 2011; Pachlopnik Schmid et al., 2011). The prognosis is similarly poor for XLP2 without HCT, in which mortality is attributed to HLH (30%), colitis (23%), liver failure (8%), and infectious causes (8%) (Pachlopnik Schmid et al., 2011).
HLH is generally treated with corticosteroids, cyclosporine, and etoposide. Rituximab has been used successfully to prevent EBV-induced FIM in XLP1 (Milone et al., 2005), and should be considered in any XLP1 or -2 patient who experiences primary EBV infection.
Lymphomas can be effectively treated with standard chemotherpateutic regimens; however, patients should be carefully monitored for the development of EBV and other infections, which can be difficult to manage due to underlying immune defects.
Patients with hypogammaglobulinemia are treated with monthly immunoglobulin replacement.
Asymptomatic patients with XLP should be periodically monitored for immunoglobulin levels, evidence for EBV exposure, and signs of development of other manifestations of disease.
HLH is generally treated with corticosteroids, cyclosporine, and etoposide. Rituximab has been used successfully to prevent EBV-induced FIM in XLP1 (Milone et al., 2005), and should be considered in any XLP1 or -2 patient who experiences primary EBV infection.
Lymphomas can be effectively treated with standard chemotherpateutic regimens; however, patients should be carefully monitored for the development of EBV and other infections, which can be difficult to manage due to underlying immune defects.
Patients with hypogammaglobulinemia are treated with monthly immunoglobulin replacement.
Asymptomatic patients with XLP should be periodically monitored for immunoglobulin levels, evidence for EBV exposure, and signs of development of other manifestations of disease.
Genes involved and Proteins
Note
XLP1. SH2D1A consists of 4 exons spanning 25 kb of genomic DNA and encodes a 128 amino acid protein comprised primarily of a Src Homology 2 (SH2) domain. Over 70 disease-associated mutations have been identified (Filipovich et al., 2011).
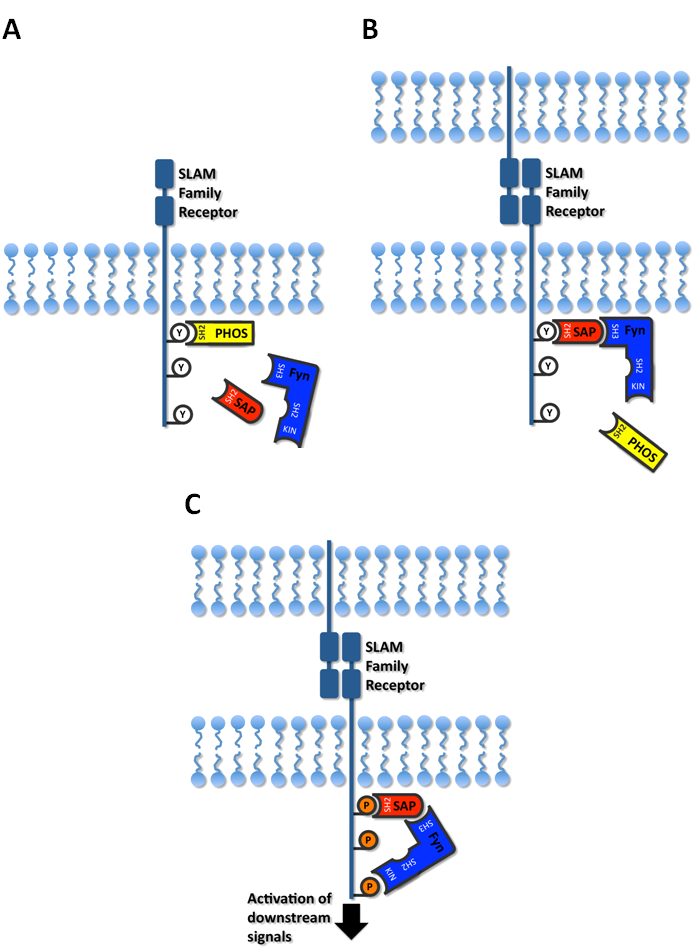
Schematic representing the putative mechanism of SAP-mediated signaling. (A) In the absence of SAP, signaling from the SLAM family receptors is impaired due to the binding of inhibitory phosphatases, such as SHP-1, SHP-2 or SHIP. Via a unique portion of its SH2 domain, SAP binds to the Src family tyrosine kinase Fyn, which leads to the activation of Fyns kinase activity. (B) Engagement of SLAM family receptors via homotypic or heterotypic interactions with similar receptors on neighboring cells leads to a conformational change in the SLAM receptor tails, thereby facilitating the binding and SAP and Fyn. (C) Fyn then phosphorylates specific tyrosines within the SLAM receptors, which form docking sites for additional signaling proteins, and allow the transmission of signals required for cell functions, such as Th2 type cytokine production, cytotoxicity and natural killer T cell development.
Note
XLP2. XIAP consists of 6 exons spanning 42 kb and encodes a 497 amino acid protein. The XIAP protein contains 3 Baculovirus IAP Repeat domains and a C-terminal Ring domain with E3 ubiquitin ligase activity. XIAP binds the tumor necrosis factor receptor-associated factors TRAF1 and TRAF2 and inhibits apoptosis through interactions with caspases 3, caspases 7, and caspases 9. It is still unclear how mutations in XIAP and the resulting disinhibition of apoptosis result in the manifestations of XLP2.
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 20926771 | 2011 | X-linked lymphoproliferative disease due to SAP/SH2D1A deficiency: a multicenter study on the manifestations, management and outcome of the disease. | Booth C et al |
| 9771704 | 1998 | Host response to EBV infection in X-linked lymphoproliferative disease results from mutations in an SH2-domain encoding gene. | Coffey AJ et al |
| 20301580 | 1993 | X-Linked Lymphoproliferative Disease. | Meyer L et al |
| 12437631 | 2002 | X-linked lymphoproliferative disease: clinical, diagnostic and molecular perspective. | Gaspar HB et al |
| 20489057 | 2010 | XIAP deficiency: a unique primary immunodeficiency best classified as X-linked familial hemophagocytic lymphohistiocytosis and not as X-linked lymphoproliferative disease. | Marsh RA et al |
| 15494422 | 2005 | Treatment of primary Epstein-Barr virus infection in patients with X-linked lymphoproliferative disease using B-cell-directed therapy. | Milone MC et al |
| 21119115 | 2011 | Clinical similarities and differences of patients with X-linked lymphoproliferative syndrome type 1 (XLP-1/SAP deficiency) versus type 2 (XLP-2/XIAP deficiency). | Pachlopnik Schmid J et al |
| 4852784 | 1974 | Letter: Fatal infectious mononucleosis in familial lymphohistiocytosis. | Purtilo DT et al |
| 21083659 | 2011 | X-linked lymphoproliferative syndrome: a genetic condition typified by the triad of infection, immunodeficiency and lymphoma. | Rezaei N et al |
| 17080092 | 2006 | XIAP deficiency in humans causes an X-linked lymphoproliferative syndrome. | Rigaud S et al |
| 9774102 | 1998 | The X-linked lymphoproliferative-disease gene product SAP regulates signals induced through the co-receptor SLAM. | Sayos J et al |
External Links
Citation
Hamid Bassiri ; Kim E Nichols
X-linked lymphoproliferative disease (XLP)
Atlas Genet Cytogenet Oncol Haematol. 2012-04-01
Online version: http://atlasgeneticsoncology.org/cancer-prone-disease/10028/x-linked-lymphoproliferative-disease-(xlp)
