Nervous System: Neurofibroma
2007-04-01 Lan Kluwe , Christian Hagel , Victor Mautner Affiliation1.Laboratory for Tumor Biology, Developmental Disorders, University Hospital Eppendorf, Martinistr. 52, 20246 Hamburg, Germany.
Summary
Classification
Classification
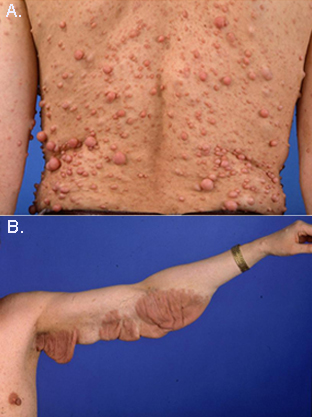
Dermal neurofibromas are well circumscribed solid cutaneous tumors with limited size.
Plexiform neurofibromas (PNF) originate from subcutaneous or visceral peripheral nerves and involve multiple fascicles extending along the length of a nerve.
In contrast to dermal neurofibromas, plexiform neurofibromas vary in size and can be extremely large. Multiple dermal neurofibromas are the hallmark of neurofibromatosis type 1 (NF1), an autosomal dominant genetic disease with an incidence of approximately 1 in 3000. Plexiform neurofibromas develop in approximately 30% of NF1 patients. While dermal neurofibromas also occur in non-NF1 patients, PNFs are almost exclusively associated with NF1.
Clinics and Pathology
Embryonic origin
Etiology
Epidemiology
Clinics
However, dermal neurofibromas usually do not cause any further serious dysfunction. There is no evidence for malignant transformation of dermal neurofibromas.
In contrast, PNF often lead to pain, disfigurement, neurological and other clinical deficits. PNF mostly show net-like growth pattern along nerve roots extending from a main nerve root to a small distal branch, and can be divided into two main types: internal tumors and superficial ones.
Superficial PNF do not cross tissue planes and are amenable to complete or nearly complete surgical resection.
Internal PNF extend through multiple tissue planes and can not be completely removed in most cases without damaging tissues and organs. PNF located in the chest, abdomen or pelvis are frequently detected as paraspinal masses that involves multiple spinal levels. These tumors may also appear as anterior mediastinal masses, sciatic nerve lesions with pelvic extension, and perirectal plexiform and uterine tumors, all leading to sever clinical complications. Furthermore, there is a risk of malignant progression in PNF, especially the internal ones. While dermal neurofibromas mostly appear during adolescence, PNF are mainly congenital though some of them become apparent later. Growth of PNF is slows down with increasing age.
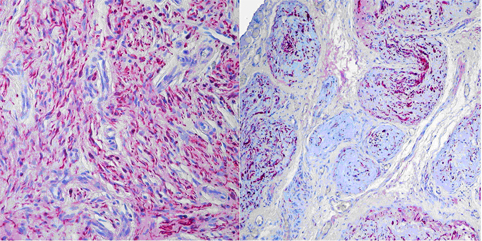
Pathology
Some cases may show a mixed Schwannoma-neurofibroma differentiation, these tumours are termed Schwannoma in Neurofibroma.
Immunohistochemical labelling of tumour cells with antibodies against S-100 protein is particularly helpful in tumours with extremely low cellularity like in dermal neurofibromas of the mamilla.
Treatment
Hormones: Hormonal factors seem to contribute to the growth of neurofibromas, as neurofibroma growth is stimulated by puberty and pregnancy. A recent study has shown that 75% of neurofibromas carry progesterone receptors. However, there is no evidence that progesterone and combined oral contraceptive pill stimulate growth of neurofibromas. For pregnant NF1 patient, obstetrician and clinicians should be aware that spinal and pelvic neurofibromas may progress rapidly and thus need to be monitored closely.
Plexiform neurofibromas: Deeply located tumors PNF often lead to pain and neurological deficits and thus need special attention and closely monitoring. Patients developing deficits or pain should undergo surgery whenever a positive outcome is suggested. Annual examination helps to detect first indication of possible spinal cord compression. Regular MRI is important for early detection of malignant transformation.
Results of surgery of PNF are usually unsatisfactory because of the network-like growth of the tumors often involve multiple nerve fascicles and other adjacent tissues. Typically surgical interventions for PNF are restricted to debulking procedures of large tumors causing significant clinical complications or aesthetic disfigurement. However, successful subtotal resections of the superficial PNF with significant improvement in cosmetic appearance are possible. Furthermore, a recent study reported the advantage of early surgical intervention of small PNF in children under 15 years of age. Total resection was achieved in all 7 cases without causing any neurological or organic deficit. Annual control within four years with magnetic resonance tomography did not reveal any relapse of the tumors.
Prognosis
Cytogenetics
Note
Genes Involved and Proteins
Gene name
Location
Note
Dna rna description
Protein description
Germinal mutations
Somatic mutations
Neurofibromas are composed mainly of Schwann cells and fibroblasts. By selectively culturing Schwann cells and fibroblasts, respectively, from an neurofibroma, is has been demonstrated that the somatic NF1 alterations only exist in the former but not in the later cell type. These results provided genetic evidence that Schwann cells are the progenitor tumor cells in neurofibromas.
Result of the chromosomal anomaly
Note
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 16000167 | 2005 | Concurrent chemoradiotherapy with low dose weekly gemcitabine in stage III non-small cell lung cancer. | Abacioglu U et al |
| 2121371 | 1990 | The NF1 locus encodes a protein functionally related to mammalian GAP and yeast IRA proteins. | Ballester R et al |
| 2114220 | 1990 | A major segment of the neurofibromatosis type 1 gene: cDNA sequence, genomic structure, and point mutations. | Cawthon RM et al |
| 11239415 | 2001 | NF1 tumor suppressor gene function: narrowing the GAP. | Cichowski K et al |
| 7550323 | 1995 | Benign neurofibromas in type 1 neurofibromatosis (NF1) show somatic deletions of the NF1 gene. | Colman SD et al |
| 15694151 | 2005 | Subtotal and total resection of superficial plexiform neurofibromas of face and neck: four case reports. | Friedrich RE et al |
| 10451710 | 1999 | Loss of NF1 allele in Schwann cells but not in fibroblasts derived from an NF1-associated neurofibroma. | Kluwe L et al |
| 5279523 | 1971 | Mutation and cancer: statistical study of retinoblastoma. | Knudson AG Jr et al |
| 15655144 | 2005 | Prevalence of neurofibromatosis 1 in German children at elementary school enrollment. | Lammert M et al |
| 16117837 | 2005 | Adenocarcinoma in bladder diverticulum, metastatic from gastric cancer. | Matsuhashi N et al |
| 16432718 | 2006 | MRI growth patterns of plexiform neurofibromas in patients with neurofibromatosis type 1. | Mautner VF et al |
| 12591720 | 2003 | Progesterone receptor expression in neurofibromas. | McLaughlin ME et al |
| 9326316 | 1997 | Confirmation of a double-hit model for the NF1 gene in benign neurofibromas. | Serra E et al |
| 11115850 | 2000 | Schwann cells harbor the somatic NF1 mutation in neurofibromas: evidence of two different Schwann cell subpopulations. | Serra E et al |
| 9633723 | 1998 | CT imaging in adults with neurofibromatosis-1: frequent asymptomatic plexiform lesions. | Tonsgard JH et al |
| 14722917 | 2004 | Characterization of the somatic mutational spectrum of the neurofibromatosis type 1 (NF1) gene in neurofibromatosis patients with benign and malignant tumors. | Upadhyaya M et al |
| 1694727 | 1990 | Deletions and a translocation interrupt a cloned gene at the neurofibromatosis type 1 locus. | Viskochil D et al |
Citation
Lan Kluwe ; Christian Hagel ; Victor Mautner
Nervous System: Neurofibroma
Atlas Genet Cytogenet Oncol Haematol. 2007-04-01
Online version: http://atlasgeneticsoncology.org/solid-tumor/5098/nervous-system-neurofibroma
