Bone: Osteoblastoma
2009-02-01 Carlos Eduardo de Andrea , Pancras CW Hogendoorn Affiliation1.Department of Pathology, Leiden University Medical Center, P1-30, Albinusdreef 2, 2333 ZA Leiden, The Netherlands
Summary
Note
Osteoblastoma (OB) is defined as a rare benign bone forming neoplasm which produces woven bone spicules, which are bordered by prominent osteoblasts (WHO, 2002).
This tumour was first described in 1932 by Jaffe and Mayer in a case report of an osteoblastic osteoid tissue-forming tumor of a metacarpal bone. It was been reported under various names, such as osteogenic fibroma of bone and giant osteoid osteoma. Subsequently, in 1956, it was given its current name, when Jaffe and Lichtenstein independently proposed the term benign osteoblastoma.
This tumour was first described in 1932 by Jaffe and Mayer in a case report of an osteoblastic osteoid tissue-forming tumor of a metacarpal bone. It was been reported under various names, such as osteogenic fibroma of bone and giant osteoid osteoma. Subsequently, in 1956, it was given its current name, when Jaffe and Lichtenstein independently proposed the term benign osteoblastoma.
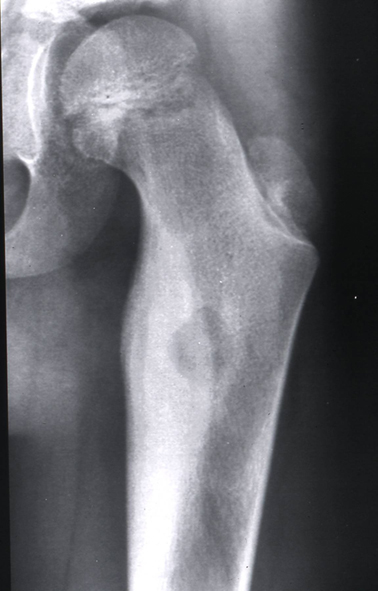
Osteoblastoma. Well delineated, radiolucent/radiopaque lesion.
Clinics and Pathology
Etiology
The genetic cause of OB has not been established but there is a report of an unbalanced translocation resulting in the loss of the chromosome 17 short arm. MDM2 amplification was reported in one case and TP53 deletion at a splice region was demonstrated in an aggressive OB. Other reports described that recurrence was statistically correlated with p53 protein expression and high PCNA index.
Epidemiology
OB accounts for approximately 1% of all bone tumors. The tumor most commonly involves the vertebral column, particularly the posterior or dorsal elements, as well as the diaphyses of long bones, pelvis, talus, facial bones, and short bones of the hands and feet.
Most of the patients affected by OB are in the second or third decades of life.
Males are affected more commonly than females.
Most of the patients affected by OB are in the second or third decades of life.
Males are affected more commonly than females.
Clinics
Swelling, pain and tenderness are usually the general symptoms of OB.
The clinical presentation of the spine tumours may include back pain, scoliosis and myelopathic and/or radicular symptoms, and suggest a herniated disc.
The clinical presentation of the spine tumours may include back pain, scoliosis and myelopathic and/or radicular symptoms, and suggest a herniated disc.
Pathology
OB is usually round to oval with a thinned cortex. If the cortex is destroyed always a thin periosteal reactive bone shell is found. Usually this tumour has an extremely rich vascular supply.
Microscopically, OB is characterized by woven bone trabeculae and osteoid, lined by a prominent, single layer of osteoblasts, and an intervening hypocellular but highly vascular stroma.
The osteoblasts are usually uniform and cytologically bland; however, about 10% of cases may be composed predominantly of epithelioid osteoblasts often proliferating in a multifocal pattern.
The differentiation between OB and osteosarcoma (OS) is one of the most challenging problems in Orthopedic Pathology. OBs are often progressive tumours with a propensity for locally aggressive growth. Approximately 25% of patients have radiographic and histologic aspects that may suggest malignancy, such as epithelioid osteoblasts, bizarre cells, mitosis, and lace- or sheet-like osteoid production. The entity aggressive osteoblastoma was introduced by Dorfman and Weiss (1984) and Lucas et al.(1994) to describe lesions with features borderline between osteoblastoma and osteosarcoma. In OS cases, a permeative pattern of growth within intratrabecular spaces and a lack of maturation toward the periphery of the lesion have been described. The term aggressive osteoblastoma designates a tumor with local destructive behavior, but without metastatic potential.
Microscopically, OB is characterized by woven bone trabeculae and osteoid, lined by a prominent, single layer of osteoblasts, and an intervening hypocellular but highly vascular stroma.
The osteoblasts are usually uniform and cytologically bland; however, about 10% of cases may be composed predominantly of epithelioid osteoblasts often proliferating in a multifocal pattern.
The differentiation between OB and osteosarcoma (OS) is one of the most challenging problems in Orthopedic Pathology. OBs are often progressive tumours with a propensity for locally aggressive growth. Approximately 25% of patients have radiographic and histologic aspects that may suggest malignancy, such as epithelioid osteoblasts, bizarre cells, mitosis, and lace- or sheet-like osteoid production. The entity aggressive osteoblastoma was introduced by Dorfman and Weiss (1984) and Lucas et al.(1994) to describe lesions with features borderline between osteoblastoma and osteosarcoma. In OS cases, a permeative pattern of growth within intratrabecular spaces and a lack of maturation toward the periphery of the lesion have been described. The term aggressive osteoblastoma designates a tumor with local destructive behavior, but without metastatic potential.
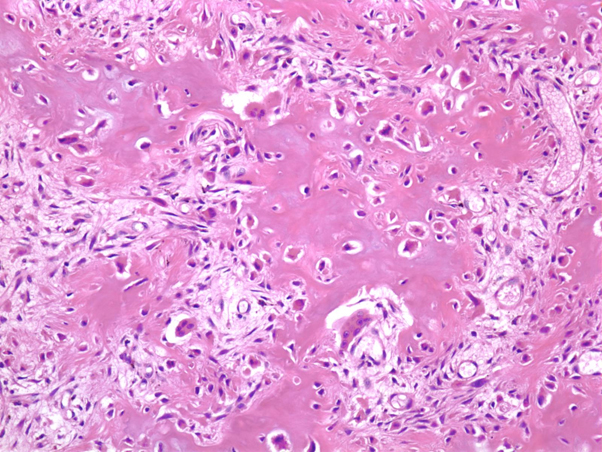
Osteoblastoma. Consisting of anatomosing woven bone trabeculae, lined by a single but prominent layer of osteoblasts, and intervening hypervascular, hypocellular intertrabecular spaces.
Treatment
When possible, en bloc resection is the therapy of choice.
Prognosis
OB is a benign bone tumor with a recurrence potential as high as 22%. However, malignant transformation has been reported in rare cases and occurs in less than 1% of cases.
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 8302813 | 1993 | Osteoblastoma-like osteosarcoma. The Rizzoli Institute experience. | Bertoni F et al |
| 3855268 | 1985 | Osteosarcoma resembling osteoblastoma. | Bertoni F et al |
| 6600112 | 1984 | Borderline osteoblastic tumors: problems in the differential diagnosis of aggressive osteoblastoma and low-grade osteosarcoma. | Dorfman HD et al |
| 16897210 | 2006 | Premalignant conditions of bone. | Horvai A et al |
| 16822878 | 2007 | Utility of immunohistochemical analysis for cyclo-oxygenase 2 in the differential diagnosis of osteoblastoma and osteosarcoma. | Hosono A et al |
| 17052641 | 2006 | Osteoblastoma of the maxilla and mandible: a report of 24 cases, review of the literature, and discussion of its relationship to osteoid osteoma of the jaws. | Jones AC et al |
| 8119712 | 1994 | Osteoblastoma: clinicopathologic study of 306 cases. | Lucas DR et al |
| 8374902 | 1993 | Unbalanced translocation resulting in the loss of the chromosome 17 short arm in an osteoblastoma. | Mascarello JT et al |
| 17505702 | 2007 | Classical osteoblastoma, atypical osteoblastoma, and osteosarcoma: a comparative study based on clinical, histological, and biological parameters. | Oliveira CR et al |
| 9820862 | 1998 | Genetic instability in osteoblastic tumors of the skeletal system. | Radig K et al |
| 16544339 | 2006 | Fine-needle aspiration of spinal osteoblastoma in a patient with lymphangiomatosis. | Rhode MG et al |
Citation
Carlos Eduardo de Andrea ; Pancras CW Hogendoorn
Bone: Osteoblastoma
Atlas Genet Cytogenet Oncol Haematol. 2009-02-01
Online version: http://atlasgeneticsoncology.org/solid-tumor/5343/bone-osteoblastoma
