Bone: Osteoid Osteoma
2009-02-01 Carlos Eduardo de Andrea , Pancras CW Hogendoorn Affiliation1.Department of Pathology, Leiden University Medical Center, P1-30, Albinusdreef 2, 2333 ZA Leiden, The Netherlands
Summary
Note
Osteoid osteoma (OO) is defined as a benign bone-forming tumour characterized by small size, limited growth potential and disproportionate pain (WHO, 2002). Usually, OO is solitary, although the literature shows few reports of multiples lesions in the same patient, but not concomitant.
In most cases, OO patients complain of severe nocturnal pain that usually responds to salicylates and nonsteroidal anti-inflammatory drugs (NSAIDs). The exact mechanism of the pain in OO and why it is more intense at night is still unknown. Some reports have shown that the nidus is responsible for the severe pain, as evidenced by the disappearance of pain when the nidus is completely excised, and that prostaglandins seem to play a major role. Prostaglandin E2 is believed to prompt vasodilation and pain. An increase concentration of prostaglandin has been found in the nidus of the lesion, as well as, a strong positivity for cyclooxygenase-2 (a key enzyme in the production of prostaglandins, particularly prostaglandin E2).
In most cases, OO patients complain of severe nocturnal pain that usually responds to salicylates and nonsteroidal anti-inflammatory drugs (NSAIDs). The exact mechanism of the pain in OO and why it is more intense at night is still unknown. Some reports have shown that the nidus is responsible for the severe pain, as evidenced by the disappearance of pain when the nidus is completely excised, and that prostaglandins seem to play a major role. Prostaglandin E2 is believed to prompt vasodilation and pain. An increase concentration of prostaglandin has been found in the nidus of the lesion, as well as, a strong positivity for cyclooxygenase-2 (a key enzyme in the production of prostaglandins, particularly prostaglandin E2).

Osteoid Osteoma. Showing dense surrounding reactive sclerotic bone.
Clinics and Pathology
Etiology
The pathogenesis of OO remains controversial. Some hypotheses have been reported:
OO is a real neoplasm; OO is a reactive process that arises on an inflammatory basis; OO is an unusual healing and reparative process. However, this tumour does not enlarge, seldom exceeds 1cm in greatest diameter; and in some cases, spontaneous regression and healing occur. Contrary to typical neoplasms, the nidus of OO contains a relatively immature central area with more mature calcified peripheral bone.
Epidemiology
OO is the third most common benign bone tumor. Its incidence is 11% among the benign tumors and 3% among all primary bone tumors. It is most common in the second and third decades. There is a male to female preponderance of 3 to 1.
The majority of the OO cases occur in lower extremity of long bones, particularly in the proximal femur. In the spine, they almost exclusively occur in the posterior vertebral elements. Additionally, OOs may occur in a juxtaarticular bone within a synovial cavity where they are termed intraarticular OOs. They are typically located in diaphyseal or metaphyseal cortices, but may rarely be located in the medullary cavity or periosteum. Infrequently, they are seen in the epiphysis.
The majority of the OO cases occur in lower extremity of long bones, particularly in the proximal femur. In the spine, they almost exclusively occur in the posterior vertebral elements. Additionally, OOs may occur in a juxtaarticular bone within a synovial cavity where they are termed intraarticular OOs. They are typically located in diaphyseal or metaphyseal cortices, but may rarely be located in the medullary cavity or periosteum. Infrequently, they are seen in the epiphysis.
Clinics
Characteristically, patients complain of localized pain, generally worse at night and relieved with salicylates. This classic presentation is not always present and, however, night pain may be observed with other bone tumours. More importantly, virtually all patients have progressive pain.
The natural history of untreated OO is toward spontaneous regression, it is taken an average of 6 years. During this period, the nidus gradually begins to calcify; afterwards, ossify, and, finally, blends into sclerotic surrounding bone. The local pain gradually diminishes.
Indication for surgery depends on symptom severity and the patients pain tolerance. With surgical resection, it has been emphasized that nidus removal is essential for pain relief.
Familial occurrence of OO is an exceedingly rare event. The literature has reported only two descriptions of OO occurring in two siblings (Kaye and Arnold, 1977; Kalil and Antunes, 2003).
The natural history of untreated OO is toward spontaneous regression, it is taken an average of 6 years. During this period, the nidus gradually begins to calcify; afterwards, ossify, and, finally, blends into sclerotic surrounding bone. The local pain gradually diminishes.
Indication for surgery depends on symptom severity and the patients pain tolerance. With surgical resection, it has been emphasized that nidus removal is essential for pain relief.
Familial occurrence of OO is an exceedingly rare event. The literature has reported only two descriptions of OO occurring in two siblings (Kaye and Arnold, 1977; Kalil and Antunes, 2003).
Pathology
Morphologically, OO is a well-circumscribed lesion, consisting of a central area of woven bone trabeculae and osteoid, lined by a prominent single layer of plump osteoblast, and an intervening hypocellular but highly vascular stroma. The bone trabeculae are irregularly arranged and thin. Hyaline cartilage is not present. Osteoclasts may be distributed randomly throughout the lesion. Significant mitotic activity is usually absent and, when preset, limited to the stromal cells. Mature OO may be composed virtually entirely of compact woven bone. In all cases, the nidus is sharply demarcated from the surrounding, generally sclerotic bone.
The nidus of OO usually has 1.5 to 2 cm in size and consists of osteoid, osteoblasts, and variable amounts of fibrovascular stroma.
OConnell et al., in 1998, reported that 25 of 34 cases of OO contained phosphorylated neurofilament-, neurofilament-, and/or S-100-positive nerve fibers in the reactive zone around the nidus and/or in the nidus. The nerve fibers were larger and more abundant in the reactive zone than in the nidus, and they were occasionally visible on H&E-stained slides, on retrospective review. None of the control bone tumours (e.g., osteoblastomas, osteosarcomas, giant cell tumours) had detectable nerve fibers either within their substance or within the surrounding bone.
The nidus of OO usually has 1.5 to 2 cm in size and consists of osteoid, osteoblasts, and variable amounts of fibrovascular stroma.
OConnell et al., in 1998, reported that 25 of 34 cases of OO contained phosphorylated neurofilament-, neurofilament-, and/or S-100-positive nerve fibers in the reactive zone around the nidus and/or in the nidus. The nerve fibers were larger and more abundant in the reactive zone than in the nidus, and they were occasionally visible on H&E-stained slides, on retrospective review. None of the control bone tumours (e.g., osteoblastomas, osteosarcomas, giant cell tumours) had detectable nerve fibers either within their substance or within the surrounding bone.
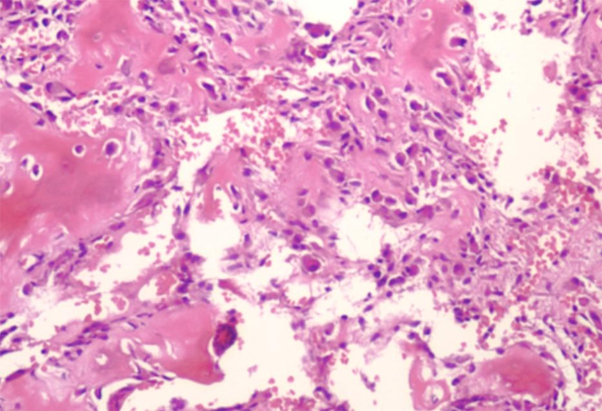
Osteoid Osteoma is characterized by anastomosing woven bone trabeculae, rimmed by a single layer of prominent osteoblast.
Treatment
After radiographic and surgical localization, the nidus should be removed in its entirety.
Prognosis
Local recurrence is rare but may occur years after the initial surgery.
Genetics
Note
Baruffi et al., in 2001, described the cytogenetic analysis of cells derived from two OO. The first tumour showed del(22)(q13.1) as the sole clonal chromosome alteration. The same alteration was present in the second OO, as a non-clonal entity. The authors mentioned that structural chromosomal alterations involving 22q13.1 in OO may affect critical genes involved in the regulation of cell proliferation, such as the YWHAH gene that codes for a 14-3-3 family members, dimeric phosphoserine-binding proteins that participate in signal transduction and checkpoint control pathways. Their primary function in mammals is to inhibit apoptosis. They also described that another gene mapped in this region is PDGFB that codes for a platelet-derived growth factor, a beta polypeptide (simian sarcoma viral [v-sis] oncogene homolog), a potent mitogen for cells of mesenchymal origin, also involved in the transformation process.
Article Bibliography
| Pubmed ID | Last Year | Title | Authors |
|---|---|---|---|
| 11172903 | 2001 | Osteoid osteomas with chromosome alterations involving 22q. | Baruffi MR et al |
| 12802523 | 2003 | Familial occurrence of osteoid osteoma. | Kalil RK et al |
| 598131 | 1977 | Osteoid osteomas in siblings. Case reports. | Kaye JJ et al |
| 16932114 | 2006 | Osteoid osteoma: a current review. | Lee EH et al |
| 9504688 | 1998 | Osteoid osteoma: the uniquely innervated bone tumor. | O'Connell JX et al |
| 9973993 | 1999 | Bone tumors of the coracoid process of the scapula. | Ogose A et al |
| 7130236 | 1982 | Two osteoid-osteomas in one patient. A case report. | Rand JA et al |
Citation
Carlos Eduardo de Andrea ; Pancras CW Hogendoorn
Bone: Osteoid Osteoma
Atlas Genet Cytogenet Oncol Haematol. 2009-02-01
Online version: http://atlasgeneticsoncology.org/solid-tumor/5342/bone-osteoid-osteoma
